Menopause is a natural phase in a woman's life, typically occurring in her late 40s or early 50s, marked by the end of menstrual cycles. It happens when the ovaries produce fewer hormones, leading to symptoms like hot flashes and mood swings. After 12 consecutive months without a period, menopause is officially diagnosed. While it's a normal part of aging, some women manage symptoms through lifestyle changes or medical interventions.
It represents a notable phase in life characterized by a notable decline in estrogen, a hormone that plays a protective role for bones and joints. More than half of individuals experiencing menopause report joint stiffness. However, connecting this life transition directly to joint stiffness is challenging due to the coincidental emergence of musculoskeletal problems during the age of menopause.
We're not sure what exactly causes frozen shoulder, and the available research doesn't strongly link it directly to menopause. However, menopause could indirectly lead to joint pain and stiffness due to issues like poor sleep, fatigue, depression, and sexual dysfunction.
Even though there's not strong evidence, it's interesting to note that frozen shoulder tends to be more common during menopause. Some experts think hormonal changes during menopause might have a role in causing it.
How to treat a Frozen shoulder
Treatment for frozen shoulder typically involves managing symptoms and improving the range of motion in the affected shoulder. Physical therapy is a key component, with specific exercises and stretches designed to enhance flexibility and strength in the shoulder joint.
Heat and ice therapy can also be beneficial for pain relief and reducing inflammation. Nonsteroidal anti-inflammatory drugs (NSAIDs) may be recommended to alleviate pain and swelling. In some cases, corticosteroid injections directly into the shoulder joint can provide short-term relief from inflammation.
Additionally, joint distension, a procedure involving the injection of sterile water into the joint capsule, may be considered to help stretch the tissue and improve mobility. Severe cases that do not respond to conservative treatments may require manipulation under anesthesia or surgical intervention to release the joint capsule and restore movement.
It is essential for individuals with frozen shoulder to work closely with healthcare professionals to determine the most suitable treatment plan based on the severity of their condition and overall health. The goal is to manage pain, enhance shoulder function, and gradually regain full range of motion over time. Patience and consistent adherence to recommended exercises and therapies are crucial components of successful frozen shoulder treatment.
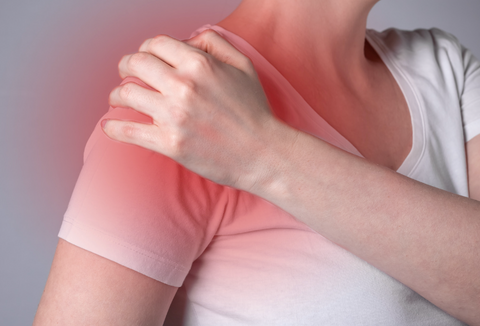
Frozen Shoulder and Dressing
When dealing with a frozen shoulder, it's a good idea to choose clothes that are loose-fitting and have a front closure to avoid putting extra strain on the affected shoulder. Opting for bras with front closures without back hooks can make dressing and undressing easier.
Soft and stretchable fabrics can also provide more flexibility and minimize irritation. It's important to communicate specific needs to caregivers or support networks to ensure a comfortable and supportive approach to dressing during the recovery process.
 Liberare front-closure bra for frozen shoulders
Liberare front-closure bra for frozen shoulders